NL Journal of Dentistry and Oral Sciences
(ISSN: 3049-1053)
The Intermaxillary Lip Bumper as a Multifunctional Appliance
Author(s) : Mohamed Youssef*. DOI : 10.71168/NDO.02.04.123
Abstract
The Intermaxillary Lip Bumper is an orthodontic appliance that associates active and functional treatment. It utilizes muscular forces to achieve the desired tooth movements and relies on the periosteal muscle tension to influence growth and stimulate subperiosteal bone apposition. Additionally, it focuses on rehabilitating muscular balance to correct dentoalveolar and skeletal disorders during the treatment of malocclusion. Tissue support is also essential for achieving the required anchorage. This appliance is removable but can be fixed when necessary. The Intermaxillary Lip Bumper is often used in conjunction with active treatment using fixed appliances, thereby reducing the overall duration of orthodontic treatment during adolescence or late growth stages. There are three main types of the Intermaxillary Lip Bumper: The Intramaxillary Lip Bumper Type I can enhance intramaxillary anchorage and space maintenance, alleviate labial pressure on the dental arch, enhance periosteal traction through the overactivity of the mental and labial muscles, and contribute to the alignment and expansion of dental arches, the Intermaxillary Lip Bumper Type II can be used to treat Class II cases caused by mandibular retrognathism, to motivate anterior rotation and anterior position of the mandible, rotating respectively along with the potential of expansion of the upper and the Intermaxillary Lip Bumper Type III, can be used to correct skeletal Class III malocclusion due to maxillary retrognathism and Class III cases caused by mesially drafted lower molars, as well as for intermaxillary anchorage. Keywords: Intermaxillary Lip Bumper, Skeletal Class III Malocclusion, Skeletal Class III Malocclusion, Skeletal Change, Mandibular Rotation, Dentoalveolar Changes, Molar Distalization, Anchorage.
Introduction
Functional appliances gained popularity in the latter half of the 20th century as a therapeutic method for growth modification in growing patients [1].
A variety of appliances have been developed, including the activator and its various modifications; the EOA and SOA as proposed by Klimt; the Bionator by Balters; the double plate designed by Schwarz; the elastic Gebissformer after Bimler; the Twin-block after Clark; the “Functions Regler” after Frankel; and ultimately, fixed functional appliances [1,2,3,4,5,6].
Numerous studies have demonstrated the effectiveness of these appliances in growth adjustment and the advancement of skeletal abnormalities in growing patients. Results have varied depending on the specific appliance used, the type of malocclusion, and the associated facial growth patterns [7,8,9].
Many studies have evaluated the effectiveness of functional treatment of Angle’s Class II/1 malocclusion and have demonstrated that removable functional appliances can effectively advance the mandible. However, this forward movement of the mandible is associated with a backward rotation, which reduces the aesthetic improvement despite achieving a normal occlusal relationship [7].
Furthermore, research indicates that a common side effect of using fixed and removable functional appliances to treat Angle’s Class II/1 malocclusion is the protrusion of the lower incisors, which occurs because the appliances exert pressure on the lower dental arch [7,8,9,10].
Frankel constructed his appliance, “Functions Regler,” to utilize tissue anchorage and periosteal muscle strain, stimulating bone apposition according to Roux’s principle. He applied osteoperiosteal traction in functional therapy by directing and correcting muscular activity, proposing that osteoperiosteal formation could occur through the muscular traction of the periosteum, particularly in cases of mandibular retrognathism with a horizontal growth pattern. He integrated labial bumpers into his appliance to alleviate labial pressure on the dental arch and enhance periosteal traction through the overactivity (tension) of the mental and labial muscles. Suggesting the increased tension on the periosteum to promote bone deposition along the anterior edge of the mandibular alveolar crest. Additionally, the tongue musculature would be free to act on the anterior segment of the mandible, facilitating equilibrium around the dentoalveolar complex [5,10]. The purpose of bumpers in the FR-II appliance is to relieve destructive labial muscular pressure on the dental arch, allowing for normal sagittal growth of dental and skeletal components of the mandible. This process also aims to achieve an equilibrium in tongue muscular tension [5,10,11]. This technique aimed to establish functional balance and promote bodily tooth movement. However, the size of the appliance has limited patient acceptance and wearability, highlighting the critical role of the patient’s cooperation in the success of orthodontic treatment.
Furthermore, addressing skeletal disorders often requires a two-phase approach: correcting the skeletal issues and managing the related dentoalveolar disorders. This strategy can extend the overall duration of treatment.
On the other side, the conventional Lip bumpers have been utilized alongside fixed orthodontic appliances for many years to achieve various objectives, including controlling anchorage, maintaining space, improving the activity of the labial muscles, increasing dental circumference, relieving crowding, and addressing lower lip sucking or biting habits [12,13].
The mechanism of lip bumpers involves disrupting the muscle equilibrium between the labial and tongue muscles, favoring the latter. This results in lateral and anterior expansion of the dental arch, along with corresponding dental movements in the same direction.
Lip Bumper has been tested on the maxilla, where they were applied with the Lip Bumper modified to extend deep into the buccal vestibule in conjunction with the Utility arch to enhance anchorage and expand the intermolar distance, similar to the Headgear. This modification showed good results in widening the maxillary intermolar space and preventing intrusion (Youssef 1995, figure 1).
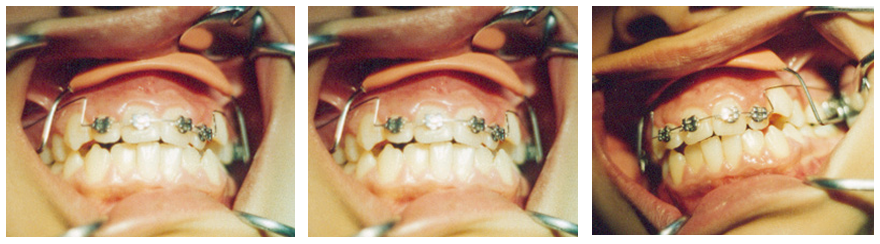
Figure 1: Modified Lip Bumper.
Our initial modifications to lip bumpers (Hallaj and Youssef in 2006) involved positioning labial bumpers in the depth of the buccal vestibule while allowing their use in combination with fixed orthodontic appliances through the molar bands on the mandible. This modification demonstrated significant dentoalveolar and skeletal changes [14].
The Appliance encourages forward positioning of the mandible in Class II malocclusions and stimulates mandibular growth to correct the intermaxillary relationship. This method operates independently of mandibular dentoalveolar anchorage, which may help reduce the overall treatment duration for malocclusions (figure 2).
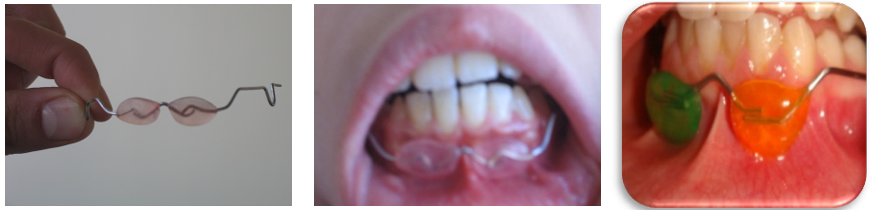
Figure 2: Modified Lip Bumper (Youssef & Hallaj 2006)/ Intramaxillary Lip Bumper; IMLB Type I
Based on the background mentioned, the Intermaxillary lip Bumper was introduced (Youssef and Al Dumaine, 2011) as a new appliance that utilizes muscular traction of the subperiosteum for functional therapy. This device positions the mandible anteriorly in class II cases, prompting anterior mandibular growth and thus correcting the distal intermaxillary relationship. Importantly, this mechanism does not rely on mandibular dentoalveolar anchorage. Additionally, it can be applied alongside fixed appliances during orthodontic treatment, potentially reducing the overall duration of treatment [15].
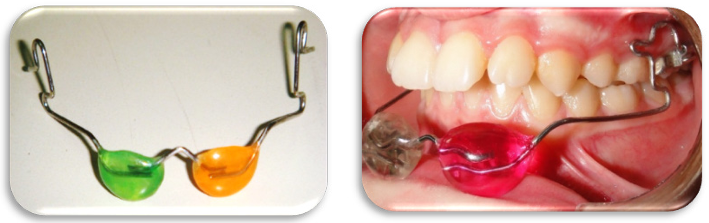 Figure 3: The Intermaxillary Lip Bumper after Youssef and Al Dumaine, 2011, IMLB type II
Figure 3: The Intermaxillary Lip Bumper after Youssef and Al Dumaine, 2011, IMLB type II
Numerous clinical cases demonstrated mandibular advancement, decreases of overjet, correction of canine and molar relationships, and improvement of facial profile during the treatment with Inter Maxillary Lip Bumper (figure 4).
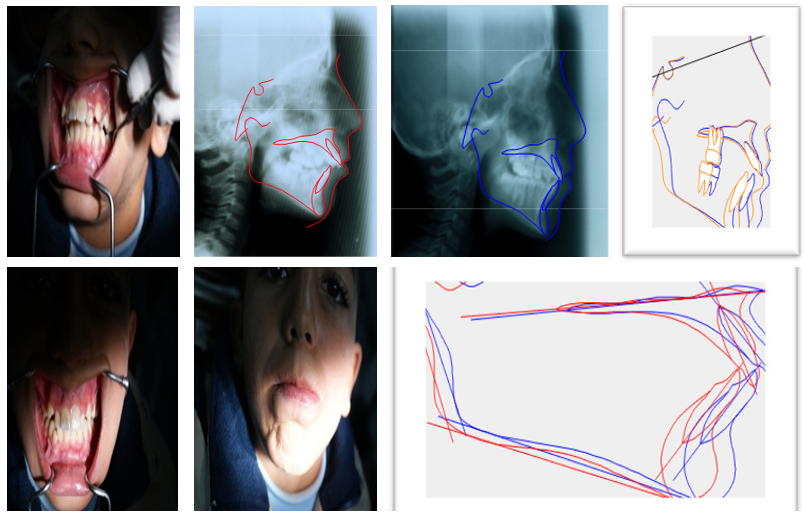 Figure 4: Patient R.S. was treated with IMLB type II
Figure 4: Patient R.S. was treated with IMLB type II
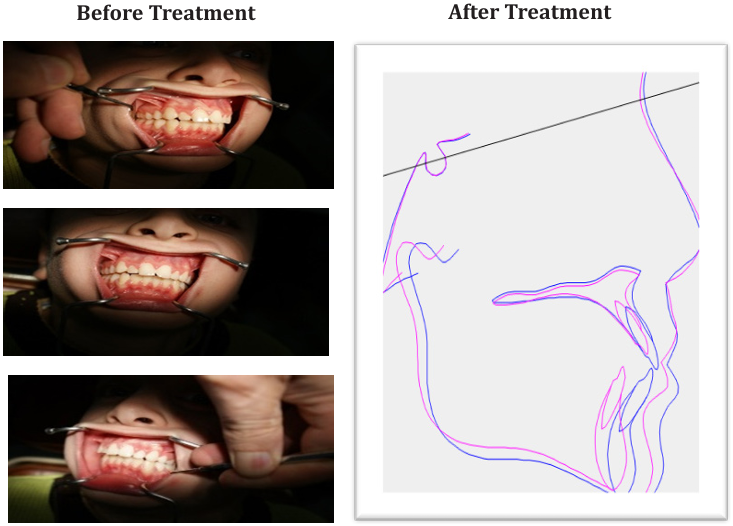
Figure 5: Patient B.M. was treated with IMLB type II
A preliminary study evaluated the skeletal and dentoalveolar changes resulting from the treatment of Class II/1 malocclusion with the Intermaxillary Lip Bumper [16]. The study involved analyzing lateral cephalograms of nine patients (five males and four females) with Cl. II/1 malocclusion treated with the intermaxillary lip bumper. In total, 18 lateral cephalograms were assessed, concentrating on 18 reference variables. The data obtained were subjected to statistical analysis using the t-test to identify significant differences between measurements taken before and after treatment. The comparison between after and before-treatment showed significant differences in the following variables: the sum of the angles after Bjork, Co-Pog., N-s: spp, N-S: Go-Me, B, SNB, ANB, SNPog, L Lip: E Line, and U1: N-S.
The results revealed that the “Intermaxillary Lip Bumper” can improve the mandibular position and rotation, jaw relationship, facial growth type, facial profile, adjustment of the Molar relationship, and the Incisor axis [16].
A Randomized controlled trial was performed to evaluate the effectiveness of the Intermaxillary Lip Bumper in the Class II/1 malocclusion treatment compared with the Activator [17,18,19].
The study contained 40 (21 female and 19 male) patients with class II/1 malocclusion divided into two groups; the first group,20 patients (11 male, 9 female), received an Activator, while the second group, 20 patients (10 male, 10 female), were treated with the Intermaxillary Lip Bumper. Pre- and post-treatment cephalograms and dental cast models were evaluated by measuring 25 cephalometric dental and skeletal measurements, in addition to the intermolar widths, arch length, Overjet, overbite, and arch depth, which were measured on the cast models.
The results showed that the Intermaxillary Lip Bumper and the Activator are sufficient to treat the skeletal Class II/1 malocclusion. However, the Intermaxillary Lip Bumper is more effective for advancing the mandible, while the Activator has more impact on the maxilla.
The Intermaxillary Lip Bumper promotes anterior mandibular rotation, contrary to what occurs with the treatment with the Activator and other removable functional appliances [18,19].
The impact of the Intermaxillary Lip Bumper on the upper and lower incisor areas is less pronounced than that of the Activator and other removable functional appliances.
The Intermaxillary Lip Bumper can be more recommended for treating Class II malocclusion cases due to retrognathic with posterior rotation of the mandible and cases of incisor protrusion.
The treatment with the Intermaxillary lip bumper led to a slight increase in the intermolar width of the upper and lower dental arch, nevertheless, the treatment with Activator led to a reduction in intermolar width, arch depth, and an increase in arch length. Overjet and overbite were reduced significantly, as correction resulted from the growth modification in the treatment of both devices [17,19] (figure 6).
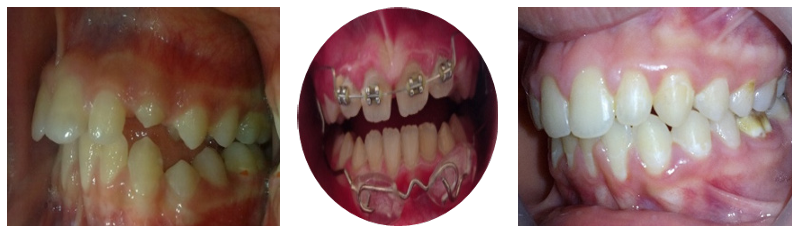
Figure 6: The Treatment Stages in the IMLB Group
Securing anchorage is one of the most significant challenges facing orthodontists when treating various malocclusions. Skeletal Class II malocclusion is at the forefront of malocclusions, which can be treated with different procedures and techniques, including elastics and fixed and removable functional appliances, particularly in adolescents. However, most of these approaches exhibited a loss of anchorage, which reduces the skeletal modifications needed to achieve facial and functional perfection [20]. The control of anchorage improves both aesthetic and functional outcomes for patients. Anchorage loss during the Class II malocclusion treatment usually manifests as protrusion and labial inclination of the lower incisors [7]. Researchers have attempted to control the position of the incisors in various ways, with some resorting to splints, others by enveloping and bandaging many of the teeth. With the proliferation of orthodontic mini-screws, attempts to utilize skeletal anchorage to achieve anchorage control arose. On the other hand, some researchers used devices that do not affect anchorage by not resting on the teeth, such as Frankel’s Function Reger and the Intermaxillary Lip Bumper. The effectiveness of both the Intermaxillary Lip Bumper and mini-screw was evaluated in a Randomized Controlled Trial conducted to assess the Role of mini-screws and the Intermaxillary Lip Bumper in the Anchorage Reinforcing during the Treatment of Class II Malocclusion with fixed orthodontic Appliances in adolescents [20]. The Trial also aimed to detect the major skeletal and dentoalveolar changes resulting from this treatment.
The study included 60 patients (aged 12 to 14 years) treated with fixed orthodontic appliances. The participants were at the end of the alignment and leveling phase randomly divided into three equal groups (in the first group, an Intermaxillary Lip Bumper was applied, and indirectly anchored intermaxillary elastics were placed on two mini-screws in the mandible between the roots of the first and second lower molars and attached to the adjacent first molar collar using a bonding wire). In the third group, traditional intermaxillary elastics were applied. Treatment continued until the alteration of the sagittal occlusal relationship.
The evaluation was performed clinically, radiographically, and on plaster casts.
The results indicated that the mandible advanced in the three groups, with the most significant advancement observed in the Intermaxillary Lip Bumper group, followed by the intermaxillary mini screws anchored elastics, and the least advancement in the traditional intermaxillary elastic group.
Regarding the maxilla, there was a decline in both elastic groups, while a slight advancement was found in the intermaxillary lip Bumper group. Therefore, the correction of the skeletal abnormality in the sagittal direction was similar between the Intermaxillary Lip Bumper and mini-screw anchored elastics group. But significantly different from the traditional intermaxillary elastics group.
The mandibular incisor protrusion was significant in the traditional intermaxillary elastics group, while this protrusion was very limited in the Intermaxillary Lip Bumper and mini screws anchored elastics groups.
Regarding vertical growth patterns, the Intermaxillary Lip Bumper group maintained its growth pattern modifications throughout anterior rotation of the mandible and light posterior inclination of the maxilla, while the vertical dimension increased slightly in the two elastic groups.
When comparing the amount of skeletal correction, the Intermaxillary Lip Bumper and the mini screws anchored elastics groups achieved more than 70% of the correction, whereas this achievement is only about a third of the total correction in the traditional elastics group.
The Overjet decreased, the intermolar relationship was corrected, and the arch widths, especially in the upper jaw, increased significantly in the three groups without significant intergroup differences [20].
Based on the results of these studies, it can be concluded that the Intermaxillary Lip Bumper, when combined with fixed orthodontic appliances to treat patients with Class II malocclusion in adolescents, can effectively enforce the mandibular arch, can lead to significant skeletal changes, stimulate the mandibular growth, can control vertical growth and posterior rotation of the mandible, have a limited effect on maxillary growth and do not inhibit or restrain the anterior maxillary growth, can maintain the degree of incisor tilt and is more effective in improving the patient’s overall profile.
The Intermaxillary Lip Bumper can shorten treatment time compared to two-phase Class II skeletal treatments (figure 7).
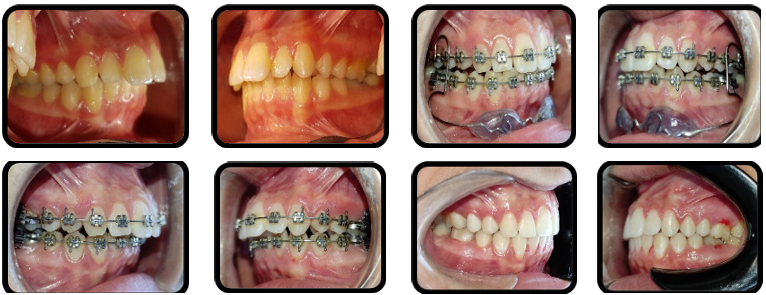
Figure 7: The Treatment Stages in the IMLB Group
In class II/1 cases caused by the medially drafted and rotated upper molars, the Intermaxillary Lip Bumper can be used to distalize and rotate the upper molar, respectively, along with the potential of expansion of the upper arch through the reflex action of the lower lip in response to the action of the lip bumper (figure 8). In situations where the distalization of the upper molars is not desired, the Trans-Palatal Arch (TPA) can be utilized.
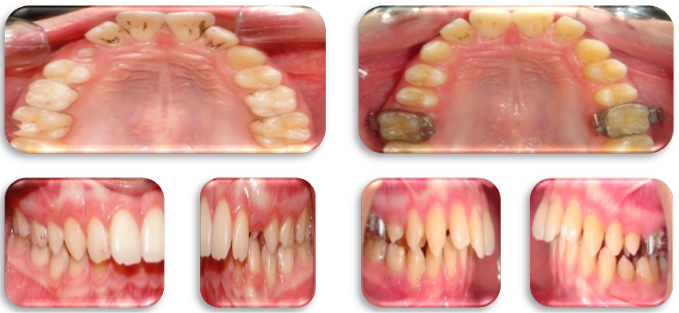
Figure 8: Distalization of the upper molal with IMLB type II
The Intermaxillary Lip Bumper can be used to treat cases of class III malocclusion due to retrognathic maxilla by reversing its use as the appliance is inserted into orthodontic bands attached to lower permanent first molars, where the lip bumpers are positioned in the upper buccal vestibule (figure 9).
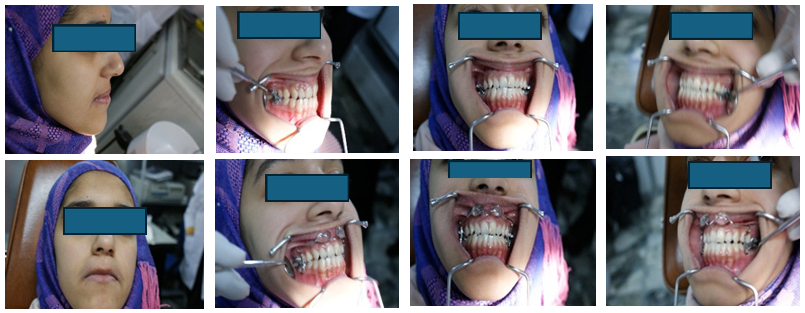
Figure 9: Patient with class III malocclusion treated with IMLB type III
A Randomized Controlled Trial was conducted to evaluate the effectiveness of the modified Intermaxillary Lip Bumper in treating patients with Class III malocclusion compared to the mandibular retractor [21].
The study included 34 patients aged 9th -12th years with skeletal class III malocclusion. The patients are divided into two groups. The first consisted of 17 patients (12 males, 5 females) treated with Intermaxillary Lip Bumper type III. The second included 17 patients (11 males, 6 females) treated with a removable mandibular retractor. Lateral cephalograms and cast study models were taken before and after treatment. Many linear and angular measurements were analyzed to assess skeletal, dentoalveolar, and soft tissue changes.
The results exhibited an improvement in the sagittal intermaxillary relationship resulting from significant anterior movement of point A and increased SNA angle, significant posterior movement of Points B and Pog., protrusion of the maxillary incisors, significant retrusion of the mandibular incisors, improvement of the Overjet, decrease of the nasolabial angle, and significant increase of the facial convexity angle. It also moves point A significantly forward, contributing correction of the existing skeletal abnormality. Treatment with Intermaxillary Lip Bumper type III can significantly improve the trajectory of the facial soft tissue profile due to the improvement in both the facial convexity angle and the nasolabial angle without changing the lower vertical dimension of the face (figure 10).
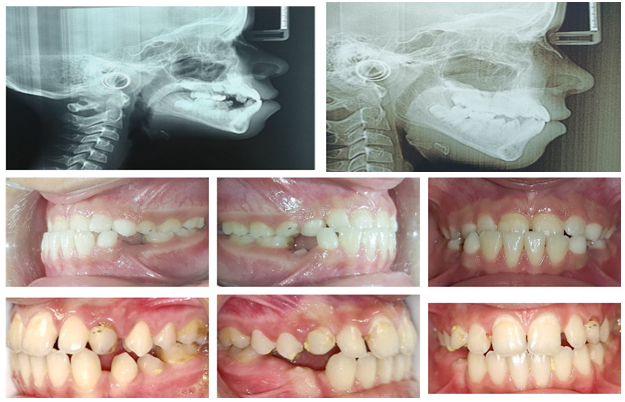
Figure 10: Patient A.S. (11 years) with skeletal Class III was treated with IMLB type III
These results revealed the effectiveness of the Intermaxillary Lip Bumper type III in correcting skeletal Class III malocclusion and its good acceptance by patients; thus, the Intermaxillary Lip Bumper type III can be considered an effective functional device in treating skeletal Class III malocclusion due to maxillary retrognathism in the late stage of mixed Dentition. Therefore, the Intermaxillary Lip Bumper type III can be recommended for the treatment of mild to moderate skeletal Class III malocclusion cases during the mixed Dentition phase.
Conclusion
The Intermaxillary Lip Bumper is an orthodontic appliance that combines active and functional treatment. It relies on muscular forces to achieve the desired tooth movements and on periosteal muscle tension to modify growth and stimulate subperiosteal bone apposition. It also depends on rehabilitating muscular balance to correct dentoalveolar and skeletal disorders during the treatment of malocclusion. It also relies on tissue support to achieve the desired anchorage. It is a removable appliance and can be fixed when necessary.
They can be used alongside active treatment with fixed appliances and reduce the duration of orthodontic treatment. It can be used in adolescence or the late growth stages.
There are three main types of the Intermaxillary Lip Bumper:
- The Intramaxillary Lip Bumper Type I: This model is used to enhance intramaxillary anchorage and space maintenance, alleviate labial pressure on the dental arch, enhance periosteal traction through the overactivity of the mental and labial muscles, and contribute to the alignment and expansion of dental arches.
- The Intermaxillary Lip Bumper Type II: This model can be used to treat Class II cases caused by mandibular retrognathism, to motivate anterior rotation and anterior position of the mandible, and to treat skeletal Class II cases caused by the mesially drafted and rotated upper molar by rotating respectively along with the potential of expansion of the upper arch through the reflex action of the lower lip in response to the action of the lip bumper and as well as for intermaxillary anchorage.
- The Intermaxillary Lip Bumper Type III: This model can be used to correct skeletal Class III malocclusion due to maxillary retrognathism and Class III cases caused by mesially drafted lower molars, as well as for intermaxillary anchorage.
References
1. Profit, W., Henry., Fields, David. Sarver; “Contemporary Orthodontics” 4th Ed.Mosby, 2019.
2. Klammt, G.; Der Elastisch -Offene Aktivator. J. A. Barth Leipzig 1984.
3. Bimler, H. P.; Gebissformer, Bimler laboratoren,wiesbaden,1985.
4. CLARK, W. J. (1988). The twin block technique. A functional orthopedic appliance system. Am J Orthod Dentofacial Orthop, 93(1), 1-18. doi: 0889-5406(88)90188-6.
5. Frankel, R: Frankel R. Technik und Handhabung der Funktionsregler. VEB Verlag Volk und Gesundheit. Berlin 1984.
6. Pancherz, H. und S. Ruf; Herbst-Apparatur, in: Kieferorthopaedie II, 4.Aufl. Urban&Fischer, Muenchen Jena 2000.
7. Youssef, M.; Das Wachstumsmuster des Gesichtsschaedels und sine therapeutische Beeinflussung durch herausnehmbare, kieferorthopaedische Gerate. Inaugural -Dissertation, Rostock,1987.
8. Antanas S, Vilma S, Mantas S ; Assessment of Skeletal and Dental Pattern of Class II Division 1 Malocclusion with Relevance to Clinical Practice. Stomalologija. Baltic Dental and Maxillofacial Journal,8:3-8 2006.
9. Cozza P, Baccetti T, Franchi L, De Toffol L, McNamara J: Mandibular changes produced by functional appliances in class II malocclusion:A systematic review Am J .Dentofacial Orthop. 2006 May;129(5):599-611.
10. Frankel R.Decrowding during eruption under the screening influence of vestibular shields. Am J Orthop1974;65:372-406.
11. Janson et al. Class II treatment effects of the Frankel appliance. Eur J Orthop. 2003 Jan;25(3):301-9.
12. Attazodeh F, Adenwalla ST. A Cephalometric analysis of the clinical appliance of the lip bumper. J Dental Res 1988; 67:252.
13. Bergersen EO. A Cephalometric study of the clinical use of the mandibular lip bumper. Am J Orthop 1972; 61:478-602.
14. Hallaj H, Youssef M (supervisor); The effect of modified lip bumper on the subperiosteum bone growth in anterior lower area. (Master thesis) Damascus University 2006.
15. Mohamed Youssef, and A. Doumani; “Intermaxillary Lip Bumper” International PCT Patent; Pub. No: wo/2011/159261, Pub. Date: 22/12/2011.
16. Youssef, M. (2012). The Treatment of Skeletal Class II-Malocclusion with “INTERMAXILLARY LIP BUMPER”. IADR/LAR, Iguaçu Falls, Brazil, 2012.
17. Kayali1,S., M. Youssef; Evaluation of dentoalveolar changes following functional treatment in-patient with class II division I malocclusion-using Intermaxillary Lip Bumper in comparison with Activator: A randomized clinical trial Azerbaijan Medical Journal, Volume 63, Issue 11, November 2023.
18. Kayali1,S., M. Youssef; The effectiveness of the Intermaxillary Lip Bumper in the treatment of Class II/1-malocclusion compared with the Activator: A Randomized controlled trial.
19. Kayali, S., M. Youssef (Supervisor); Evaluation of Intermaxillary Lip Bumper Effectiveness during the Treatment of Skeletal Class II- cases (Randomized Control Trial) A dissertation submitted in fulfilment of the requirements for (Ph.D.) in Orthodontic & Dentofacial Orthopedics- Damascus University 2023.
20. Alkhalaf, R., M. Youssef ( supervisor); The Role of Miniscrews and the Intermaxillary Lip Bumper in the Anchorage Rein forcing during the Treatment of Class II – Malocclusion with Fixed orthodontic Appliances in Adolescences -(Randomized Control Trial). A dissertation submitted in fulfilment of the requirements for (Ph.D.) in Orthodontic & Dentofacial Orthopedics- Damascus University- 2025.
21. AL-Saleh, Q., M. Youssef (Supervisor); Evaluation the efficiency of modified intermaxillary lip bumper in treatment of skeletal class III-cases -Randomized Controlled Trial A dissertation submitted in partial fulfilment of the requirements for the degree of Master in Orthodontics and Dentofacial Orthopedics, Damascus University- 2022.
This article licensed under the Creative Commons Attribution 4.0 International License CC-BY 4.0., which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are properly credited.
